Even now, three years after COVID-19 first appeared, nothing is understood about how it causes serious illness, particularly the extensive organ damage that goes beyond only the lungs. Scientists are discovering more and more that damage to the blood arteries leads to organ malfunction, but it is unknown why the virus causes this harm. The crucial molecular pathway has now been found, according to a multidisciplinary team of Emory researchers.
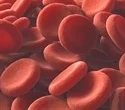
Their study’s findings, which were just published in Nature Communications, demonstrate that COVID-19 harms the cells lining the tiniest blood veins, preventing blood flow. These findings may open the door to novel therapies that could prevent the daily deaths of hundreds of patients from COVID-19.
Drs. at Emory Healthcare began this investigation in the early stages of the pandemic, physicians at Emory Healthcare began this study to learn more about the causes of severe COVID-19 and the reasons why adults experience severe illness more frequently than children. They compared the blood biochemistry of COVID patients to that of non-COVID patients using a method known as “multi-omics,” which involves evaluating many data sets simultaneously. This finding, according to Maier, was especially intriguing considering their clinical observations that the blood from COVID-19 patients who were seriously unwell was exceptionally viscous—imagine maple syrup instead of water.
Wilbur Lam, an associate professor in the Department of Pediatrics at Emory University as well as the Wallace H. Coulter Department of Biomedical Engineering at Georgia Institute of Technology and Emory University, was Maier’s partner and co-senior author.
They were able to see how blood from COVID-19 patients would flow in the human body differently than blood from other patients thanks to the creation of state-of-the-art models of the smallest blood arteries, which are predicted to be the most susceptible to altered blood flow. Viewing the movies from these microfluidic devices, according to Maier, is similar to watching how COVID-19 might be changing our blood arteries in real time. “Endothelial cells, which are actual human vascular cells, coat these artificial blood vessels. Red blood cells, plasma, or any other essential blood component can be added, along with various combinations, to observe how the blood functions and how damage develops.”